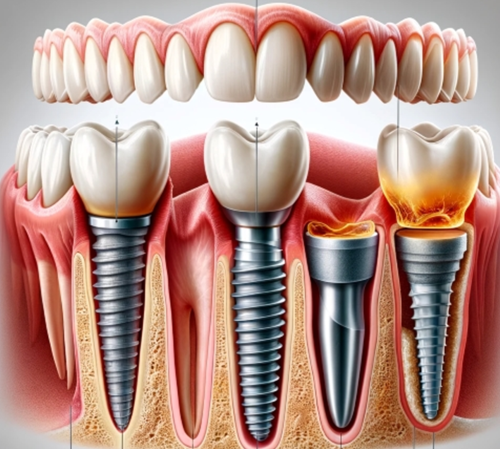
Titanium-zirconium alloy has emerged as a promising alternative to pure titanium for oral implants, offering several advantages due to its enhanced mechanical properties and biocompatibility. This alloy, typically comprising about 13-15% zirconium with the balance being titanium, combines the desirable characteristics of both metals, making it an attractive material for dental implantology.
Advantages of Titanium-Zirconium Alloy over Pure Titanium:
- Increased Strength: The addition of zirconium to titanium increases the alloy’s tensile strength, making it stronger than pure titanium. This increased strength allows for the production of narrower implants with the same or higher resistance to mechanical stress, which is particularly beneficial in situations with limited bone volume.
- High Biocompatibility: Both titanium and zirconium are known for their excellent biocompatibility, crucial for dental implants. The titanium-zirconium alloy maintains this property, ensuring good osseointegration and minimal risk of allergic reactions.
- Enhanced Durability: The alloy’s improved mechanical properties contribute to a longer lifespan of the implants under the dynamic and static loads of mastication, potentially reducing the risk of implant failure.
- Corrosion Resistance: Like pure titanium, the titanium-zirconium alloy exhibits excellent corrosion resistance, which is vital for maintaining the integrity of the implant in the corrosive environment of the human body.
Clinical Applications:
The titanium-zirconium alloy is especially beneficial for patients with limited bone density or when small-diameter implants are needed due to anatomical constraints. Its increased strength compared to pure titanium allows for the use of narrower implants without compromising performance, making it an ideal choice for challenging dental restorations.
Research and Outcomes of Titanium-Zirconium Alloy:
- Background: Titanium (Ti) is a preferred material for orthopedic and dental implants due to its excellent bone integration and corrosion resistance. Recent studies suggest a titanium-zirconium (TiZr) alloy, with 13–17% zirconium, may offer superior mechanical properties for high-load-bearing implants, but research is limited.
- Objective: To compare the mechanical properties and microstructures of TiZr alloy and commercially pure titanium (Ti).
- Methods: Pure Ti and TiZr alloy discs were analyzed through nanoindentation, electron dispersive spectroscopy (EDS), X-ray diffraction (XRD), and electron backscatter diffraction (EBSD).
- Results: The TiZr alloy demonstrated a significantly lower elastic modulus and higher hardness compared to pure Ti. Microstructural analysis revealed the presence of the alpha phase in both materials, with TiZr displaying a finer grain size.
- Conclusion: The TiZr alloy’s lower elastic modulus, increased hardness, and refined microstructure suggest it is more suitable for high-load-bearing implants than pure Ti. This could lead to better long-term outcomes for implants due to improved mechanical performance and potential for enhanced biological response. [1]
Conclusion:
While pure titanium remains a gold standard in dental implantology, the titanium-zirconium alloy offers significant advantages, particularly in terms of strength and suitability for specific clinical scenarios. Its use as an alternative to pure titanium for oral implants represents an advancement in dental materials, providing options for more challenging cases and potentially improving patient outcomes.
However, the choice between pure titanium and titanium-zirconium alloy should be based on specific patient needs, anatomical considerations, and clinical judgment. For more information, please visit Advanced Refractory Metals (ARM).
Reference:
[1] Sharma A, Waddell JN, Li KC, A Sharma L, Prior DJ, Duncan WJ. Is titanium-zirconium alloy a better alternative to pure titanium for oral implant? Composition, mechanical properties, and microstructure analysis. Saudi Dent J. 2021 Nov;33(7):546-553. doi: 10.1016/j.sdentj.2020.08.009. Epub 2020 Aug 29. PMID: 34803299; PMCID: PMC8589587.